Articles by Author | Articles by Topic
Impulsivity and Its Bioenergetic Relationship to ADHD
Peter A. Crist, M.D
Reprinted from the Journal of Orgonomy, Vol. 29 No. 2
The American College of Orgonomy
Distractibility, restlessness, and impulsivity are often seen in children. As problems, they are the most common presenting symptoms in children brought to mental health professionals (1). Through the years this symptom constellation has been given various designations including minimal brain damage, minimal brain dysfunction, hyperkinetic syndrome, and attention deficit disorder. Many of these children are now given the diagnosis of attention-deficit/hyperactivity disorder (ADHD).
ADHD is currently receiving widespread attention from psychiatrists, neurologists, psychologists, educators, parents, and the general public. Millions of dollars are being spent on research (2). The popular press has seen numerous books and articles including several magazine cover stories in recent years [Footnote 1] (3). Yet, with all that has been written and scientifically presented, the debate continues as to the cause and most effective treatment of ADHD. Is ADHD a psychological or a physical disorder? Are these children sick or just especially lively normal youngsters? Is the problem inherent in the children or is it the result of faulty upbringing, in particular the parents failure to discipline them (nature vs. nurture)? Does the diagnosis of ADHD even represent a true disease entity? Among the numerous observations and opinions, however, it is generally accepted that impulsivity is one of the key problems in those given the label ADHD.
Before we accept new diagnostic terms such as ADHD, it would be valuable to first review well-established knowledge. Reich's landmark study of the impulsive character more than seventy years ago stands applicable today as a solid basis from which to understand the emotional dynamics of impulsivity (4). A review of Reich's later work on biopathies and the relationship between emotions and the autonomic nervous system will help further ground our understanding of a disorder that is indeed biological, a product of disturbed energy functions.
The case of a child treated with medical orgone therapy will provide a focus for a general discussion of the characterological and bioenergetic understanding of impulsivity and its relationship to ADHD. We can also see how this therapeutic approach compares to standard treatment, which almost invariably includes the medication Ritalin [Footnote 2] in combination with behavioral therapy.
Case Presentation
J was evaluated at age six and a half at the end of his kindergarten school year. His adoptive parents were concerned about a long pattern of behavior problems both at home and in school. The problems were evident even before preschool, but in kindergarten they became more noticeable. He was disruptive, restless, and inattentive in class. At home he failed to listen to his parents, was disrespectful, arrogant, and frequently lied. If he wanted something, he would just take it. He had been caught with valuable items taken from his father's locked desk and money from his mother's purse. He was quite clever at locating his parents' keys without their knowing it. He was also found with toys belonging to other children, which he claimed had been given to him at school or when he visited on play dates. Most of these explanations were revealed to be fabrications.
J was also willful. If he wanted to do something, he would just do it. For example, if he was told to wait before going outside to play, he would go out anyway. If stopped, he would sneak out the back door or get angry and yell, throw things and slam the door. He often became angry, especially when thwarted, and acted it out in spiteful, disruptive ways. As long as he got his way there were no major blow-ups, but he was always restless. His parents said he was also sweet, helpful, and affectionate at times. They did not trust this side of his nature, however, attributing his good behavior to attempts at manipulation of them.
On occasion he was capable of sustained attention to activities of his own choosing. A careful review of how he behaved, and under what circumstances, revealed his willful, self-centered behavior to be related to his failure to control his impulses, especially those that were aggressive and gratification-seeking. He rarely showed genuine feeling for anyone else.
J was adopted at birth. There were no known physical problems during the pregnancy and delivery. He passed the usual milestones of physical development at or slightly ahead of time. Emotionally and temperamentally, however, his adoptive mother reported he always seemed immature, demanding, and impatient. For example, when J was an infant she made sure to have a bottle with her at all times because he would throw a tantrum or put up a great fuss if not attended to immediately. When he was a toddler and preschooler, she always carried cookies or juice for him because even as he got older he threw tantrums if hungry or thirsty.
The family consisted of father, mother, and younger adopted sister. The father was a busy, workaholic, corporate executive with serious heart disease. He was rarely at home except when his medical problems forced him to take time off. As a practical, no-nonsense businessman, he was quite skeptical about the value of therapy. The mother, an active homemaker with many other responsibilities, was very involved in the children's daily activities.
The parents were polarized in their attitudes toward J. The father imagined the worst and said that if J was acting like this now what would happen when he entered adolescence? He feared J would become involved in drugs or alcohol, and end up in jail. "If he is stealing from us and from kids at school now, what criminal behavior will he be doing later?" He found J's behavior incomprehensible because it was so different from his own hardworking, law-abiding attitude as a youngster. He just wanted J's problems fixed so that they would no longer disrupt the family and the peace and quiet he wanted in his only refuge from his hectic work life. He was inclined to be critical, harsh, and arbitrary in assigning punishments, but was often not around to enforce them. Meanwhile, the mother, trying to be understanding, often made excuses for J and was lenient with him. She usually thought he was just a lively kid who would outgrow his bad behavior.
Her disciplinary style allowed J's behavior to continue until she was provoked. She would then scream at him. She often threatened a consequence for his behavior but failed to follow through in the face of confrontation and J's angry outbursts. Contained in the parents' understanding of J's behavior and their methods of trying to cope with it were rational elements: the father wanted to stop J's neurotic behavior and the mother wanted to make emotional contact with him. To complicate matters further, as is not at all uncommon, the parents had significant unresolved marital tensions which often prevented them from cooperating with each other. Instead, they tended to argue about whose approach was right. Both acknowledged that J's behavior was better when he was alone with his father. The father cited this as evidence that he was handling J better than she. The mother cited this as evidence that J needed his father around more. (One of her own marital complaints was her husband's unavailability.) With his energy, persistence, perceptiveness and cleverness, J could play this lack of a unified approach to his advantage.
From age five to six and a half they had taken him to a number of psychologists and other mental health professionals, but felt these interventions had had little effect. Most recently he had been seen by a pediatric neurologist who diagnosed attention-deficit hyperactivity/disorder (ADHD) and recommended that he be started on Ritalin. Both parents wanted another opinion. The mother in particular was uncertain about using medications and wanted an evaluation to explore what else might be done.
On initial evaluation J was a bright, lively boy with an "in charge" attitude. He spoke to me as if he were interviewing me. He began to talk more rapidly and with pressured speech whenever I tried to pin him down on any subject or get him to tell his feelings. He was intense, engaging, and expressive but emotionally cool and aloof. He also had a glib, tough-guy, con man facade. Though not in touch with his emotions, he was driven by disturbing feelings. For the most part this was anxiety, although outwardly he showed very little discomfort. I had the impression he was constantly and acutely aware of my reactions to everything he said. His mind was quick and he spoke with great authority, but rapidly changed from subject to subject, often without clear direction. When asked about any of his emotions, his thinking became circumstantial and even tangential but with a controlled and controlling quality. His emotional expressions were lively and changeable but lacked warmth and human connection. When asked factual questions, he could pay attention, concentrate well, and remember details adequately. However, when asked about his relationship with the family or related matters, he became distracted and turned his attention elsewhere. His intelligence was estimated to be above average. He demonstrated no evidence of other cognitive function deficits. In this first evaluation session he was generally well-behaved except for his excessive tendency to take charge of the situation.
When told to lie on the treatment couch, he briefly appeared puzzled and uncomfortable. He quickly regained his composure, sat cross-legged in the middle of the couch, and began talking nonstop. With a mature manner and using adult words he told me about plans for the trees, shrubs, and gardens at their new house and of all his talks with the landscape architect. I again told him to lie down and he briefly did so while giving me a wary glance. A hint of anxiety showed momentarily in his eyes. He immediately popped back up to a seated position and began telling me about various sporting activities he liked to do. After repeated attempts to have him lie down by asking, then telling, and then demanding that he do so, I finally pushed him back gently and kept him recumbent by gentle nudges with my hand whenever he tried to sit up. Uncomfortable and fidgety, he crossed and uncrossed his arms and legs.
On biophysical examination, his eyes had a challenging expression. They were mobile when he looked about the room but when asked to track my finger as I moved it about, he had some difficulty. He was often ahead of my moving finger and tried to anticipate where it would go. His occiput was tense and tender. He had moderate armor in the muscles of his jaw. His voice had a tight, strained, somewhat hoarse quality. He held his neck stiffly with considerable tension in his sternocleidomastoid muscles. He tended to hold his chest in the inspiratory position but it moved adequately when he breathed. The intercostal muscles were very ticklish especially under his arms. He had marked tension and moderate hypertrophy of the thoracic paraspinal musculature. His abdomen was tense and ticklish. His pelvis was held rigidly His legs had normal muscle bulk but were somewhat tense and ticklish. He was agile and quick in his movements despite the extensive holding throughout his body.
Course of Therapy
Individual medical orgone therapy was begun with the goal of help-ing J make better contact with his warded-off emotions and improv-ing his ability to attend and concentrate. He also needed to become more aware of the consequences of his actions in order to rein in his impulsivity. It was quite evident that he deflected his feelings through constant motion and distraction. Treatment would require that J come to focus and discharge the deeper emotions he was avoiding but also partially relieving with his "hyperactive" behavior.
To accomplish this it was important to stop his contactless discharge of energy which manifested physically in restlessness and fidgeting, and behaviorally in the sneaky con man way he expressed himself. For example, when he was told to lie still on the treatment couch with his arms and legs relaxed and straight, he often sat up, taking charge, or would sneakily cross his legs or arms. To address this behavior, I either pointed out his acting the boss or his sneakiness. I also actively took control by telling him what to do, pushing him down, or holding him still.
On the couch, he was usually either unable or unwilling to lie still. When I physically restrained him to stop his movement, he initially became anxious and then quickly angry. I had him express the anger by giving me angry looks, hitting and kicking the couch, and punching a bolster-like device around my arm. He expressed a combination of genuine emotion and the attitude that this was just a game. I encouraged him to get out his negative feelings toward me and therapy, and he expressed them indirectly by refusing to do what I asked of him.
After several months of therapy which proceeded in this fashion, his mother reported that he avoided being alone, always wanted the light on at night, and frequently came into the parental bed. She said even though he seemed afraid of the dark and of being alone, he never said he was afraid but instead had various rationalizations for his behavior. During this time, his tough-guy, "I'm the boss" attitude in therapy intensified. He said in a provocative tone, "You can't tell me what to do." He also continued to be sneaky and with "I dare you" looks, crossed his legs, or put his hand under his head, often defying me when told to do something. When asked to breathe, he usually gave me a sly look and sometimes pumped his chest in a forced mechanical manner.
This resistance intensified in the several sessions that followed. I again held him still without allowing any movement. He struggled against my restraint, became more frustrated, looked me straight in the eye and said, "I hate you." His eyes welled up with tears and he said, "You don't care about me. You're just doing this for the money. Nobody cares about me. My real mom didn't want me. My mom now doesn't listen. My dad is too busy to spend any time with me." He cried briefly and I kept my hand on his chest where I had just restrained him. He did not struggle against me or try to take my hand away, and accepted some comforting from me. He then quickly composed himself and put his shoes on while talking about some sports event, as if nothing had happened between us. His mother reported he was more calm at home for the remainder of that evening and most of the next day.
In the course of the first year of treatment J showed some improvement in his emotional contact with me in therapy and in his behavior at school, but only limited improvement at home. After a year and a half of therapy J had calmed down enough that when his father took him to a school event where he was well-behaved, a school administrator commented, "I'm glad you finally put him on Ritalin." (Note: J was never given any medication.) The father, who had been urging a trial of Ritalin because he was not convinced of significant improvement, then was able to acknowledge that perhaps there was something to the therapy. At this point the parents began reporting he had improved at home, but also noted that improvements were soon followed by a return of the original problematic behavior.
Late in his second and early in his third year of therapy a number of family stresses occurred which in the past would have precipitated a deterioration in J's behavior. In the most stressful periods his lying, temper outbursts, and aggressive behavior with his sister increased at home, but improvements at school were maintained. Once school was out for the summer he did well at camp, but old patterns surfaced whenever he was out of the structured environment of either school or camp.
J had difficulty at the beginning of third grade. He was again in trouble for disruptive behavior, calling out in class, and pushing other pupils. Consultation with the parents and his new teacher addressed these problems promptly with a behavioral (reward/punishment) approach to which he responded quickly. Throughout the year this intervention was reasonably successful in containing disruptive behavior at school. He continued to improve overall, but intermittently had the same tendency to call out in class, be easily distracted by anyone near him or by what they were doing, and to do rushed and sloppy schoolwork. In his individual therapy sessions he discharged some anger. He was negative and stubborn much of the time, but as long as he was expressing himself emotionally, and not impulsively, I felt progress was being made. At least his behavior was more controlled at home and in school. By this time he could emotionally discharge his negativity by engaging in a "No!"/"Yes!" shouting match between us.
I met jointly with J and his mother on several occasions to have him face responsibilities. When confronted, he often responded by getting up to leave the room or kicking the chair on which he was sitting. At these times I physically restrained him. He struggled against me and became hot, sweaty, and emotional. His mother noted he was calmer after these episodes. She gained the courage to be more aggressive and held him accountable at home. Occasionally she physically restrained him and he became passionately angry and expressed it directly to her. He often said hurtful things at these times such as, "I don't have to listen to you. You're not my real mom." Although these episodes were always emotionally difficult for her, she saw clearly that he calmed down afterwards and was generally more cooperative for a few hours to a few days. In therapy he occasionally said that he knew his behavior was self-defeating. I felt we were making a more consistent emotional connection and I developed more empathy with him as he now appeared to be more a troubled boy than a con man.
Family Therapy
While addressing J's impulsivity in his individual sessions, it was also essential to improve the emotional environment at home and change the family dynamics that perpetuated his behavior. To accomplish this, J's mother was seen individually. This began in the first year of J's therapy and continued throughout. In addition, intermittent sessions with the parents were held and were valuable in getting them to work together in addressing J's behavior.
Initially, the mother's therapy focused on educating her and giving practical advice about how to deal with J. She needed to learn and accept that his behavior was not just a variation of normal liveliness and that for his sake she must stand up to him. In her heart she knew both of these things to be true but did not want to believe so. This was an example of a typical pattern throughout her therapy. She usually had good instincts as to what to do but became anxious about the implications of following through. She then thought of numerous possible responses and became confused. She lost sight of the import of her original instinct and talked herself out of acting on it. J's mother either minimized his behavior or reacted to each new incident as if it were an overwhelming crisis: being aggressive with other pupils at school, stealing while on a field trip or at home, yelling out whenever he did not get his way, striking out at and being mean to his younger sister, etc. She was encouraged to look at each situation as part of an overall pattern of impulsivity that required containment but also as a discrete problem that could be addressed practically. She gradually gained perspective about J's problems and an ability to tolerate her anxiety looking at them without becoming overwhelmed. Over the course of the first months of her therapy, J's mother began to see how his impulsive behavior was aggravated whenever she gave in to his demands. She needed a great deal of encouragement to stand firm in the face of his neurotic behavior (because when she disciplined him she felt guilty that she had made him feel badly and had not made everything "good" for him).
She also came to see that rather than feel guilty for her presumed role in the genesis of J's problems, she clung to the illusion that they were not so severe. When she saw how serious they indeed were, she blamed herself for having caused them and felt she had to make up for it in some way. I told her that blaming herself and trying to make up for the past was not helpful and interfered with J taking responsibility for his actions. I encouraged her to stand up to his misbehavior because that was what she could constructively do. It also became clear to her that J was instinctively aware of her guilt and played on it manipulatively. I explained that the health in him expected and needed discipline. If it were not forthcoming he would have contempt and lose respect for her which would, in turn, fuel his neurotic arrogance and lead to further misbehavior.
Helping her to tolerate feeling guilty and seeing its destructive function led her to face the anxiety that drove her to assuage her conscience by trying to take care of everything for J. She also had to be encouraged to stand her own anxiety for allowing J to fail when he did not take responsibility for a school project. She began to see that trying to protect him from discomfort relieved him of responsibility. As she let J take more responsibility and felt more secure that her husband would spend more time with him, she no longer felt overwhelmed and became calmer. She saw how her life was consumed by taking care of J and attending to his problems. She dared to think about making a life for herself beyond child care.
Meanwhile, both parents were seen in couples therapy to help them work together in raising J. The polarization of their views on J was addressed but this was only minimally successful in overcoming the serious marital tensions between them. Their relationship was of a volatile type (5). In the first session they were shouting recriminations at each other about who was to blame for J's problems. This made it impossible to directly address their marital difficulties. To be of value, therefore, these sessions had to be kept focused on practical issues that required working together to overcome J's misbehavior.
Early on, the issue of how they were dealing with his dishonesty came up for discussion. J often spun elaborate cover-up stories for his behavior. His father wanted to punish him for his misbehavior once the truth was known. His mother wanted to be understanding and show him they trusted him in order to get him to be trustworthy. I pointed out that the lying about his misdeeds had to be dealt with before the deeds themselves were addressed, and that trust was to be earned not granted. Punishing misbehavior without first addressing the dishonesty would cause J to become sneakier and more devious in hiding his behavior. A step-by-step approach to his dishonesty was developed in my discussions with them. First, they needed to make him aware of his dishonesty by consistently telling him they did not trust him or what he said. Second, they had to encourage him to come clean about his lying by praising him when he was truthful and withdrawing a privilege when he was caught in a lie. Finally, it was essential that they wait to discipline him for misbehavior until he had been consistently honest about it. With this approach they found that he became more inclined to reveal when he had lied. By the fourth year of therapy, although he occasionally lied, he more consistently acknowledged the truth.
It was emphasized that they needed to model the behavior they expected of him. If they wanted him to be as good as his word they had to be as well. Their past actions showed otherwise. When J misbehaved, the mother tried to reason with him and then finally, out of frustration, often threatened dire consequences. Rarely did she follow through. Also, the father harangued J endlessly about present and future consequences of his misbehavior. The sheer quantity of their words rendered them ineffective.
I also informed them that if they expected J to listen to them, they had to listen to him. By the time they brought him for therapy, they no longer believed anything he said and no longer really listened to him. They were not even aware when he said something genuine. I encouraged them to pay attention to how J was saying things and to respond to that rather than to what he said. If they did not believe him, I advised them to simply tell him so. The parents were also at a loss as to how to discipline J when he was first brought to therapy. He acted unconcerned about their personal disapproval or praise. They came to see that J, a physical, quick-reacting, action-oriented person, would most likely respond to communication with similar qualities. They were advised to try, as much as possible, physically restraining him or taking immediate actions that set limits on his behavior. Verbal cajoling, long explanations, and lectures by either parent were pointed out as being of no benefit. Finally, as much as he might provoke them, physically striking him was to be avoided because this gave the message that striking out was an appropriate way to handle anger. More importantly, as a response to his provocative (masochistic) behavior, it would actually gratify his neurotic reactions.
Over the five years of J's therapy tension between his parents eased noticeably. Much of this resulted from the mother being able to respond to her emotions without reacting so intensely to her husband and from the father taking practical steps to resolve stressful complications of his work. In J's third year of therapy his father sold his company, took a partial early retirement, and began to work more from home. Only then did he begin to see and experience for himself the day today difficulties in dealing with J. He developed a better appreciation for what his wife was confronted with but still had difficulty letting go of the view that his was the best way to manage J. At the same time this change meant that he became more available and was more involved with J, disciplining him, helping with homework, and taking him to his various sporting events.
In his fifth year of therapy J, now age eleven, still acted rebelliously toward authority figures on occasion. His distrust and contempt of me as an authority figure became even more pronounced. I told him he was treating me with disrespect and that I thought he caused himself a lot of trouble by being disrespectful. He responded, "Well, I treat my parents with respect." When asked how he could say that he replied, "If I didn't they'd ground me." This made it clear that he expected to be disciplined by his parents, but remarried unaware of the quality of his behavior.
He became increasingly defiant with me while simultaneously acting more responsibly at home and in school. For a number of weeks I held him more to my expectations about lying still on the couch and called him on his attempts to sneak out of doing so. He was more fidgety and would not stop moving about. His resistance became increasingly emotional in character and he was, in effect, saying, "I won't lie still" rather than "I can't lie still." By physically restraining him at this point, a deeper defiance was brought to the surface. While restrained as much as possible, he continued at each opportunity to sneak some movement with a defiant expression on his face. I told him to just be direct and say, "No." Now he refused to even do this. He gave me his usual sly look and closed his eyes. I said, "Go on, be straight about your feelings. Say "No way, I won't,' because that's what your actions are saying." He defiantly turned his head away without a word. I managed to hold his arms with one hand and grasped his chin and moved his head back and forth in an expression of "No" while telling him, "That's it; go on and let the 'No!' out." He looked flustered, off balance, and a little anxious at not being able to control the situation.
These expressions quickly changed to a more defiant attitude. I continued to shake his head and as he resisted, I persisted. He became flushed and gave me a furious look. I encouraged him saying, "Go on. Let it come out of your eyes and mouth. Say what you want to say to me." He continued angry at me, with a greater intensity than ever, and gave me murderous glances. When I ended the session, he left seething with anger.
Later in the week the mother asked, "What did you do with J? For a day and a half after his session he kept telling me and his father about how he was angry with you and had told you how much he hated you. He was different about this than ever before. He didn't just say he wasn't coming back. He was explicit about being angry and how he told you off. He was so clear about it that I wondered what really happened." I told her, "Yes, he was angry with me but he never said a word. I think what he said to you was partly his bravado about what a brave 'big-shot' he was with me." She also reported that for the next several days after that session he was able to sit down more focused than ever and got his school work done without the usual delaying tactics and struggle with her.
The following week he promptly came into the treatment room when I called him. He lay down and spontaneously began talking to me quite openly, as one human being to another, "A lot happened this week." I replied, "Like what?" "My godfather died but I didn't know he was my godfather because I don't remember ever seeing him. He was a good friend of my parents. My mom was upset and crying all the time with red eyes and stuff. I didn't cry. I didn't really feel anything. I didn't really know him. I felt a lot sadder when my fish and my dog died. Is that weird?" I said, "No, of course not. You knew them and they meant something to you." He had not previously acknowledged sadness to me either in himself or in others. His mother later reported that he was mostly well-behaved for the rest of the week. She did say, "He drove me crazy though, by putting off a big homework project until the last minute. I have to admit that he really buckled down and worked hours and hours the two days before it was due, even though the last night his father and I were out and he was with a babysitter."
At his next session his defiance of me was back in full force. He again required physical restraint to stay still. When I persisted, he became angry again but this time was near tears by the end of the session and walked out visibly shaken. He quietly went and sat in a corner of the waiting room. Later his mother reported that she let him sit quietly for a while and then on his own he came over to her and with tears in his eyes asked for a hug. He told her I had hurt him by grabbing his jaw where he had braces. She told me he rarely came to her for comfort. I told her he was clearly upset by what had happened with me but evidently found it far easier to complain about being physically hurt than emotionally hurt. In fact, I had not applied pressure over his teeth and had held his jaw less tightly than two weeks earlier. This was an important event because he had let himself be emotionally vulnerable in asking for comfort.
At his next session he came in, lay down, and began the conversation. He said quite excitedly and proudly that he thought he would get a top grade on his next report card for the first time ever. I told him I looked forward to seeing it and he must feel good about himself. He responded quite genuinely, "Yeah, I've been doing much better at school for a few weeks. I've also been good at home. I think I've turned over a new leaf. Even my dad thinks so." Then, for the very first time, he told me of his disappointments with his parents. "They don't keep their promises. My dad is quick to promise something but then decides later to change his mind. My mom doesn't keep her promises not because she changes her mind but because she gets so distracted that she doesn't remember what she said." (Both of these observations were quite accurate.)
His mother was now reporting that he was "like a new kid." He had come to her for a hug on a number of occasions just to make physical contact. He also was well-focused on his school work. He had been promised that he could play in the intramural sports program if he got his schoolwork done. When he failed to do so the previous week and was told he could not play, he responded with disbelief, "You're not really going to keep me from playing are you?" She said it was difficult for her to hold him to their agreement because he was so upset. His response, however, was very different than other times when he did not get his way.
There were no angry outbursts and he did not become devious. Instead he told her just how much he wanted to play. She said it was the first time she ever saw him show, emotionally, that something mattered so much to him. He then got very busy and made sure that his schoolwork was done so that he would be able to play the next week.
The central theme and process of J's therapy were played out in this fashion. When his defensive actions were stopped, emotions were stirred up spontaneously. He would then lash out or assume an "in-charge-tough-guy" attitude of defiance to avoid these feelings. When he was able to experience his emotions (whether desire, anger, anxiety, or sadness) and directly express them, he calmed down and could focus on his school work or on what he needed to do to get what he wanted. The most lasting effect came when he tolerated anxiety and sadness, the emotions associated with energetic contraction. He was then able to feel genuinely good about himself and take responsibility for something that mattered to him. It also meant that he could more accurately perceive and express himself about other people (as he did about his parents).
Case Discussion
J's behaviors such as calling out, having angry outbursts, hitting his sister, lying, and stealing represented a deeply ingrained defense mechanism to prevent the development of any emotional tension. When he was first brought to therapy, his impulsive behavior was the problem that caused him most trouble at home and in school. It was also the central mechanism his character that had to be addressed in the course of his therapy. Therapeutically, the task was to bring him in contact with his underlying emotions by preventing him from behaving neurotically. He had phallic narcissistic character defenses (such as acting like a "big-shot," and trying to control everybody including teachers, parents and me), but these determined the quality of how he behaved impulsively rather than being representative of his central character structure. It is reasonably certain that his central defense of impulsivity defines his character structure as an impulsive, but because he is still a child, and has not passed through puberty, we cannot yet be sure how this will manifest in his final personality.
It appears that J's pathological character evolved from qualities that were inborn. We know from his mother's account that J was highly demanding, insistent, bright, and emotionally changeable from birth. These basic natural qualities manifested in distorted, exaggerated, and pathological form in his impulsivity, pushiness, sneaky cleverness, and conning behavior. He evidently was born with a high-energy charge and by nature was giggly reactive to internal and external stimuli. These reactions became automatic defenses against anxiety and were further reinforced by the parents' inability to cope with his intense emotional responses. It is worth noting that J did not have the dramatically chaotic upbringing often associated the impulsive character, but the amount and kind of discipline he received was evidently inadequate for his individual needs. [Footnote 3]
For more than 40 years Reich wrote, "Noisiness and biopathic hypermotility are often mistaken for natural behavior." (6) Making this distinction was more difficult with J than with other children because his ability as an actor made him an excellent con man. Discerning natural from biopathic (genuine expression from deception) requires the ability to know and sense the difference. To understand and manage children such as J, parents, teachers, and therapists must distinguish natural healthy expressions of primary impulses from secondary pathological impulsivity. J's typical behavior had an irritating, harsh quality compared to the straightforward lively expression of healthy impulses. Both of J's parents said they did not want to inhibit his natural energy and liveliness. Unfortunately this commendable desire became a rationalization for their failure to discipline his neurotic behavior. Gratifying the secondary impulses reinforced them and increased the tendency for their expression to be used defensively. On the other hand, J's parents were encouraged to support rational physical outlets for his energy and noted he was calmer at home after particularly hard workouts in soccer and baseball. [Footnote 4] (His teachers were also aware that J's behavior in class was better after an especially physical recess period.)
Theoretical Discussion
Impulsivity
Reich's landmark study of impulsivity more than 70 years ago revealed it to be not merely a moral problem, "bad character," but rather an emotional defense accessible to character-analysis. [Footnote 5]Subsequent discussion in the orgonomic literature has addressed characterological, biophysical, and therapeutic aspects of the treatment of the impulsive character. [Footnote 6] In addition to these aspects, J's case allows us to focus on some theoretical and bioenergetic issues and suggests some relationships they might have with the diagnosis of ADHD.
Reich identified the impulse-inhibited and the impulsive character as two distinct types (11). Figure1 shows Reich's general diagram of instinct and defense (12).
Figure 1
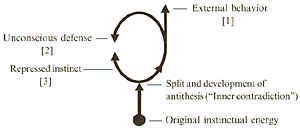
Reich illustrated this with an example of specific impulses (Figure 2) (13).
Figure 2
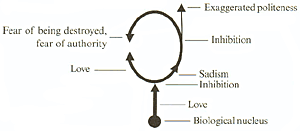
This example represents the typical impulse-inhibited or "compulsion neurotic" character. In this type, a great deal of energy is bound in the unconscious defense labeled [2] in Figure 1.
In contrast, the impulsive character engages in behavioral discharge ([1] in Figure 1) as his defense against a yet deeper impulse (Figure 3).
Figure 3
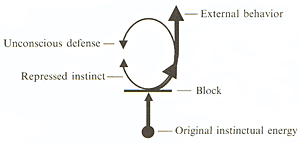
Here the energy of the defense is found more in the secondary expression ([1] in Figure 1) than in the inhibiting force. In this type, the external behavior is typically an action or an aggressive attitude (such as arrogance) rather than an inhibition or fearful attitude (such as exaggerated politeness) seen in the impulse-inhibited type.
J's emotional dynamics are like those seen in Figure 3 and can be more specifically represented as in Figure 4.
Figure 4
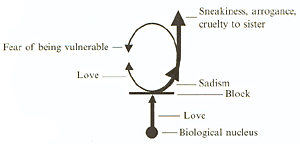
Because impulses are continually being expressed with partial energy discharge, there is less of the original repressed instinct (labeled [3] in Figure 1) bound in this type character. For example, in the inhibited type one often feels the presence of the love impulses, albeit held back and unexpressed, but J seemed very unloving until his neurotic expressions were curtailed.
Many character types demonstrate impulsivity, although it is not the central character mechanism as it is in the impulsive character. Each unsatisfied block (regardless of the stage during which it occurred) has a dynamic similar to figure 3 and a tendency toward impulsivity. [Footnote 7]
Biological Pulsation
The orgonomic concept of pulsation and its relationship to the autonomic nervous system (ANS) grounds our understanding of these emotional processes in biological functions. [Footnote 8] A biopathy can mani-fest as a tendency to be stuck either in contraction or expansion. [Footnote 9]
Charts 1 and 2 compile and organize elements of this basic antithesis in the natural and biopathic states respectively. These concepts serve to better define the bioenergetic basis of J's emotional problems and properly place them within the spectrum of biopathies.
Chart 1
Natural Pulsation
| phase of pulsation | expansion | contraction |
| associated primary emotion | pleasure | anxiety |
| predominant branch of ANS | parasympathetic | sympathetic |
Chart 2
Biopathic Disturbance of Pulsation
| biopathic state | stuck in expansion | stuck in contraction |
| intolerance of: | contraction | expansion |
| typical emotions | anger, irritability | fear, anxiety, depression |
| manner of relating | superficial contact | inhibited |
| character type | impulsive | impulse-inhibited |
| type of block | unsatisfied | repressed |
Biopathic Disturbance of Pulsation
biopathic state stuck in expansion stuck in contraction
intolerance of: contraction expansion
typical emotions anger, irritability fear, anxiety, depression
manner of relating superficial contact inhibited
character type impulsive impulse-inhibited
type of block unsatisfied repressed
J's clinical picture is consistent with the expansive, impulsive biopathy. A reactive biopathic expansion is qualitatively different from natural unarmored expansion. Because armor prevents full expansion, one would not expect to see expression of genuine emotions of love and pleasure. In J's behavior we saw non-genuine expressions of love used to con others. He often displayed anger and irritation which result from partially blocked expansive expressions turned harsh by armor. As could be predicted from J's structure, he was most intolerant of the emotions associated with contraction: anxiety, fear, and sadness.
Perception and Excitation
An orgonomic understanding of the relationship between perception and excitation is also helpful in understanding impulsive individuals. Reich identified orgonotic streaming as the common functioning principle of perception and excitation, a functional pair as expressed in Figure 5(17).
Healthy emotional contact and expression occur when energy movement is unimpeded with full integration of perception and exci-tation. "Attention deficit" and "hyperactivity" were noted by Harman to be merely descriptive terms that refer to disturbances in the paired functions in Figure 5. [Footnote 10]"Attention deficit" implies a lock of full perception "Hyperactivity" has as its source, physical excitation. If the movement of energy is relatively free-flowing but prevented from unitary emotional expression because of a perceptual disturbance, it will then be transformed into physical excitation. [Footnote 11] (See Figure 6) When J became disturbed, he discharged his tensions somatically but remained unaware of what he was feeling.
Figure 5
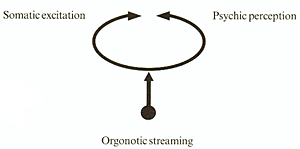
Figure 6
Preventing his physical discharge served to bring him more in contact with his emotions.
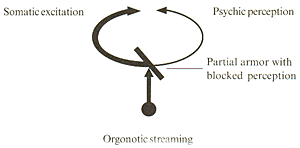
By contrast, with decreased orgonomic streaming both perception and excitation re reduced and the individual becomes emotionally deadened. (See Figure 7)
Figure 7
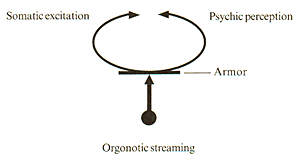
Children who suffer chronic contraction and are inhibited or withdrawn are much less likely to be identified as "difficult" than those who have impulsivity (19). Many of the more overt symptoms seen in children gradually diminish with the passage of time because further armor development and the character formation serve to reduce energy movement.
The Relationship of ADHD to Impulsivity
Most psychiatrists would diagnose J as having ADHD. Certainly, his symptoms of distractibility, impulsivity, and hyperactivity meet the criteria for this diagnosis (20). Without an understanding of the energetic basis of the symptoms, their treatment recommendations would generally include medication, such as Ritalin, and/or behavioral therapy.
ADHD research and the debate about effective treatment continue. Barkley, a prominent researcher and author in the field, has proposed a "new theory" in which he attempts to unify the many manifestations of ADHD under one psychological mechanism. He considers ADHD a "fundamental deficit in the ability to inhibit behavior" (21). This is, in reality, no more than a new name for impulsivity.
The lack of specificity of the symptoms included in the criteria for ADHD has led some professionals to question its legitimacy as a psychiatric/medical diagnosis (22). Long-term follow-up studies of patients who met criteria for a diagnosis of ADHD reveal impulsive symptomatology continuing into adult life (23). While impulsivity is the common denominator in J's character pathology, not all children with impulsive behavior develop an impulsive character. [Footnote 12] The designation ADHD lacks specificity precisely because deficits of attention with or without impulsivity may occur in many different character types, [Footnote 13] as can impulsivity itself. It appears likely, however, that a significant number of those children diagnosed with ADHD go on to develop impulsive characters.
Nature vs. Nurture
Since ancient times it has been known that primary lesions of the brain caused by trauma, infection, etc. result in secondary emotional and behavioral reactions. As early as the 1870's it was observed that frontal lobe lesions of the brain were associated with problems of impulse control. By the 1930's Kahn and Cohen noted hyperactivity with brain stem lesions and proposed the concept of "organic driveness" (25). Such observations led to the conclusion that problems of impulse control were caused solely by brain lesions. Theoreticians since have argued over whether the symptom complex now called ADHD is neurological or psychological in origin. The long list of names for this disorder reflects the numerous and changing theories about its cause.
When no gross brain lesions could be demonstrated, such problems were attributed to "minimal brain damage," that is damage that could not be detected. When more sophisticated means to evaluate brain Pathology were developed, and they still failed to find any lesions, the term "minimal brain dysfunction" was employed to account for a disturbance in function without evidence of structural brain changes. The psychoanalytically-oriented second edition of the Diagnostic and Statistical Manual (DSM-II) used the term "hyperkinetic reaction of childhood." In their effort to be purely descriptive and phenomenological (rather than attribute cause to Psychological or physiological factors), the authors of this section of the DSM-III chose the diagnostic term "attention deficit disorder" (ADD). The most current term, employed in the DSM-IV, is "attention-deficit/hyperactivity disorder" (ADHD).
Mechanistic research seeks an anatomic or physiologic basis for this disorder and regards observed structural or physiological changes as its cause, attributing these to as yet undiscovered defects that are either inborn ("genetic") or have developed since birth. The orgonomic, functional (energetic) approach is quite different. It considers characterological impulsivity a biological disorder of pulsa-tion (a biopathy) that manifests primarily in the emotional realm but which has concomitant physical changes as well. These physiologic and/or structural changes result from the underlying energy disturbance (an effect of armor) which precedes and causes them to develop in the individual. [Footnote 14] For example, a recent discovery in those diagnosed with ADHD is decreased metabolic activity of the brain's frontal lobe cortex, as demonstrated by positron emission tomography (PET) (26). The frontal lobe cortex is known to be associated with impulse inhibition and such findings of alterations in neurophysiology, without demonstrable structural change, suggest this area of the brain as a primary site of armor in this disorder. [Footnote 15] The very subtlety and variability of the physiological findings associated with the diagnosis of ADHD are more consistent with a primary emotional/energetic process than a primary physiological disorder. Some of the other physiologic findings, such as signs of excess vagal (parasympathetic) tone demonstrated in studies of heart rate variability (27) as well as studies indicating resistance to thyroid hormone (a sympathetic nervous system hormone) (28) directly support the formulation of a parasympathetic predominance of the autonomic nervous system in these cases.
The mechanistic approach creates confusion when it fails to adequately differentiate the inborn physical nature and the individual's psychological development. Articles in the popular press report patients with ADHD stating that they have a high level of energy. Individuals born with a high energy level are more prone to develop problems in an armored society because of the difficulty finding acceptable outlets for their energy. Unable to fully restrain such a child's natural impulses, the parents' partially successful attempts only lead to greater impulsivity on the part of the child.
Identical twin studies that demonstrate significant genetic factors and other research that reveals a familial pattern for ADHD are cited as proof that the disorder is inborn and biological (29). In fact, it is just as likely that particular qualities present from birth are associated with a greater likelihood of developing particular emotional pathologies. J, for example, was excitable, quick to express himself and to act right from birth. Someone with these qualities will use them defensively and will be more likely than others to become impulsive.
The Underlying Bioenergetic Basis of ADHD
A year and a half of medical orgone therapy had enabled J to calm down so noticeably that a school administrator thought he had been medicated with Ritalin. Ritalin (methylphenidate), as well as other drugs used to treat ADHD, are central nervous system stimulants. Their calming effect in the disorder is considered paradoxical because they are stimulants. One would expect, thinking "logically," that such an agent would only cause greater excitability. These agents, which include amphetamines and caffeine, also have positive effects on the other symptoms associated with ADHD. They produce the same effects as an activation of the sympathetic nervous system and are there fore termed sympathomimetic. With this in mind we are now able to form an orgonomic (energetic) hypothesis as to the true mechanism that underlies ADHD and why the disorder's symptoms are (paradoxi-cally) relieved with central nervous system stimulants. ADHD has at its root an over stimulation of the parasympathetic nervous system. In such individuals the sympathetic/parasympathetic nervous systems are not in a reciprocal balance - as they are in health. Amphetamine-like drugs offset the parasympathetic over-excitement and bring about a degree of stabilization by inducing an energetic contraction. These drugs improve the more mechanical aspects of attention disturbance (i.e., test-taking) (30). Drug treatment follow-up studies show no consistent evidence that medications improve learning or have a demonstrable long-term effect on impulsive character reactions (31).
Behavioral modification modalities make up the other common traditional therapy for ADHD. One might expect this approach, which attempts to bring about an unlearning of maladaptive behaviors, to produce some restraining effect on secondary, neurotic impulses. But such behavior modification techniques are mechanical and are not designed to help individuals come into contact with their underlying repressed emotions or provide an outlet for them. A behavioral approach cannot address the root causes of the condition any more than medications can. Medical orgone therapy, however, does just that because it takes an integrated approach to the full range of manifestations of the patient's disturbed energy functioning.
The Social Problem
Dealing with inattentive, restless, impulsive children involves much more than controlling their symptoms with medications and behavioral modification. Most people instinctively want to try to stop these children from being impulsive, at least initially. What they don't know, but find out soon enough, is that this alone is ineffective. What is required is stopping the impulsivity and helping the child to face his anxiety. While a daunting task, especially for those whose patience is lacking or has worn thin, the importance of parental involvement and attention to their children cannot be overestimated (32).
In order to help these children most effectively we must also understand the broader social context and see how it aids and abets impulsivity. [Footnote 16] Our modern society supports action and instant gratification, the quick thrill. Endless options excite and distract, but lack sustained emotional attention and connection. There is also a failure within our culture to hold individuals accountable for their actions.
In this regard, Breggin noted that the diagnosis of ADHD as it is currently used together with drug treatment has significant negative consequences (33). Telling a child he has a neurological condition, ADHD, that necessitates medication serves to absolve him and parents of responsibility for his behavior and undermines the principal requirements for genuine and lasting change. Parents must take responsibility for rationally handling their children's behavior and the child must be helped to take responsibility by making emotional contact with his actions.
Conclusion
There are no shortcuts or pills to cure the deep disturbances in the emotional structure of impulsive children. Medical orgone therapy has brought some success with this patient and with others, but it is not a panacea. J has been helped to live more with his deeper emotions. How he weathers the storms of adolescence, however, will put to the test how much has been accomplished. Impulsive children are a great challenge and require a tremendous commitment and effort on the part of family, teachers, and therapist. Although medical orgone therapy of individuals and families can reduce impulsivity and avoid the chronic character disorder seen in adult life, the greatest hope lies with preventing the development of the disorder as children mature from infancy through adolescence.
Footnotes
1. A recent computer search of an index of popular magazines showed entries for over one hundred articles about this disorder in the past two years alone.
2. Ritalin (methylphenidate) is a mild central nervous system stimulant related to amphetamine ("speed") that was found in the 1950's to have an apparently paradoxical calming effect on hyperactive children.
3. The character develops from the individual's experiences that grow out of the interaction between his individual nature and his environment and not from the specific historical events that occur. Orgonomic character diagnosis therefore is based upon an understanding of the patient's essential present-day defense mechanisms rather than deducing it from historical information.
4. The structure and discipline of these coached team sports also reinforced the needed changes in his behavior.
5. It was, in fact, Reich's work with impulsive characters that led to the development of character-analysis(7).
6. Konia (8) and Heimbach (9) reported on the treatment of adult impulsive characters. Crist reported on the treatment of impulsivity in a child who was probably a childhood impulsive character (10).
7. Baker identified two major types of emotional blocks, repressed and unsatisfied, in which either the inhibited or the impulsive tendency is confined to a specific stage of psychosexual development (14).
8. Reich conceptualized the "basic antithesis of vegetative life" and identified that pleasure and expansion are associated with the parasympathetic branch of the autonomic nervous system and anxiety and contraction with the sympathetic branch (15).
9. "Biopathy," a term coined by Reich, denotes those disease processes characterized by a primary disturbance of the biological function of plasmatic (energy) pulsation in the total organism (16).
10. Harman, R.A. In a personal communication.
11. Clinical observations support the idea that perception and excitation are heterogeneous functions that can transform into each other. See Myerowitz's explication of heterogeneous functions and their operations (18).
12. A number of children and adolescents meeting criteria for ADHD and treated in medical orgone therapy were not impulsive characters. Their individual character diagnoses included phallic, passive-feminine, and paranoid schizophrenia. They were all, however, significantly impulsive in their behavior.
13. "Deficit of attention" is a nonspecific term for perceptual problems that can range from subtle perceptual distortions associated with any of the character types (24) to severe disturbances with marked ocular armor such as those seen in schizophrenia.
14. The orgonomic understanding also includes the well-accepted observation that primary lesions of the brain have secondary effects on the behavior of the individual.
15. These findings also intriguingly suggest an antithetical relationship between frontal cortical activity and emotional expansion. We also know that cortical brain activity is associated with intellectual activity and that there is an antithetical relationship between this and sexually pleasurable expansion.
16. Editor's note: The increased prevalence of impulsive behavior among children and adolescents is one of the destructive social consequences of the breakdown of the authoritarian family structure during the past several decades. The social processes which underlie this rise in impulsivity in our society will be examined in depth in subsequent issues of the Journal of Orgonomy. CK.
REFERENCES
1. Arnold, L.E. and Jensen, P.S. "Attention-Deficit Disorders, "Comprehensive Textbook of Psychiatry (eds. Kaplan, H. and Sadock, B. J.) 6th Edition. Baltimore, MD. Williams and Wilkins, 1995,2295.
2. Goldman, E.L. "Massive Trial to Study ADHD Management, "Clinical Psychiatry News, October, 1995, 5.
3. a. Blau, M. "A.D.D. the Scariest Letters in the Alphabet," New York Magazine, 26 (49): 44-51, December 13, 1993
b. Wallis, C. "Attention Deficit Disorder: Life in Overdrive," Time, 144(3): 43-50, July 18,1994.
c. Leavy, J. "Mother's Little Helper, with Ritalin the Son Also Rises," Newsweek, March 18, 1996, 50-56.
4. Reich, W The Impulsive Character and Other Writings, (trans. Koopman, B.G.), New York: New American Library, 1974. Also published in five parts in Journal of Orgonomy, 4:4-18,149-166, 1970; 5:5-20, 124-143, 1971; 6:4-15, 1972.
5. Crist, P.A., "The Biosocial Basis of Family and Couples Therapy," Journal of Orgonomy, 2 7:166-189, 1993
6. Reich, W Children of the Future. New York: Farrar, Straus and Giroux, 1983, 66.
7. Reich, W The Impulsive Character and other Writings (trans. Koopman, B.G.). Op. Cit.
8. Konia, C. "Orgone Therapy of an Impulsive Character," Journal of Orgonomy, 3:83-91, 1969.
9. Heimbach, S. "An Impulsive Character: Problems of Diagnosis and Treatment," Journal of Orgonomy, 19:26-41, 1985.
10. Crist, P.A. "A "Problem" Child," Journal of Orgonomy, 18: 188-201, 1984.
11. Reich, W The Impulsive Character and other Writings, (trans. Koopman, B.G.). Op. Cit.
12. Reich, W Function of the Orgasm (trans. Wolfe, T.P.). New York: Farrar, Straus & Giroux, 1961, 119.
13. Ibid.
14. Baker, E.F. Man in the Trap. New York: The Macmillan Co., 1967.
15. a. Reich, W "The Basic Antithesis of Vegetative Life," (Part 1) Journal of Orgonomy, 1:4-22, 1967.
b. Reich, W "The Basic Antithesis of Vegetative Life," (Part 11), Journal of Orgonomy, 2:5-23, 1968.
c. Reich, W Function of the Orgasm (trans. Wolfe, T.P.). Op. Cit., 255-265, (summary of a. and b. above.)
16. Reich, W Cancer Biopathy New York: Orgone Institute Press, 1948, 129.
17. Reich, W Character Analysis. New York: Noonday Press, 1949, 441-442.
18. Meyerowitz, J. Before the Beginning of Time. Easton, PA: rRp publishers, 43, 45-47.
19. Crist, P.A- "A'Problem'Child," Op. Cit.,199.
20. Diagnostic and Statistical Manual of Mental Disorders, 4th edition. Washington, DC: American Psychiatric Association, 1994.
21. Barkley, R. Taking Charge of ADHD: The Complete Authoritative Guide for Parents. New York: The Guilford Press, 1995, 43-54.
22. Braughman, F.A. "Fundamentally Flawed" (letter), Clinical Psychiatry News, January, 1996, 8.
23. Arnold, L.E. and Jensen, P.S. "Attention-Deficit Disorders," Comprehensive Textbook of Psychiatry. Op. Cit., 2304.
24. a. Konia, C. "The Perceptual Function in Armoring (Part 1: General Survey," Journal of Orgonomy, 18:226-237, 1984.
b. Konia, C. "The Perceptual Function in Armoring (Part Ii: General Survey," Journal of Orgonomy, 19:122-139, 1985.
25. Kahn, E., & Cohen, L.H. "Organic Driveness: A Brain Stem Syndrome and an Experience," New England Journal of Medicine, 210:748-756, 1934.
26. Arnold, L.E. and Jensen, P.S- "Attention-Deficit Disorders," Comprehensive Textbook of Psychiatry. Op. Cit., 2298.
27. Ibid., 2300.
28. Ibid., 2298.
29. Ibid., 2298.
30. Ibid., 2304.
31. Ibid., 2304.
32. Breggin, P.R. "Q: Are behavior-modifying drugs over-prescribed for America's schoolchildren? (Symposium) Yes: Drugging our children won't cure the problems in schools," Insight on the News, I 1: 18-2 1, August 14, 1995.
33. Ibid.
